Tinea versicolor, also known as pityriasis versicolor or an-an, is a common skin condition that you can identify through the patches of skin discoloration you can see in different areas of the body. Contrary to common belief, this condition is a lot more common than you think. Having said that, this article will help you know more about its causes, symptoms, types, prevention, and cure of this skin issue.
What is Tinea Versicolor?
Tinea versicolor is a fungal infection caused by an overgrowth of yeast that naturally resides on the skin. This means that this medical condition isn’t contagious.
This condition leads to the development of discolored patches on the skin, which can be white, yellow, red, pink, brown, or tan, depending on your skin color.
It’s sometimes interchanged with vitiligo. However, vitiligo is a condition that causes smooth, light spots on the skin. On the other hand, tinea versicolor’s appearance presents as scaly patches that are not necessarily a lighter tone than the skin color of the affected person.
Causes and Risk Factors
The type of yeast responsible for tinea versicolor thrives in warm, moist, and oily environments. When constantly exposed to this habitat, it can lead to yeast overgrowth. Other factors that may contribute to this are:
- Living in tropical or subtropical climates
- High humidity and heat exposure
- Active oil glands, especially seen during puberty
- Hormonal changes due to conditions, such as hormonal imbalance and pregnancy
- Weakened immune system
Symptoms
People with tinea versicolor typically experience:
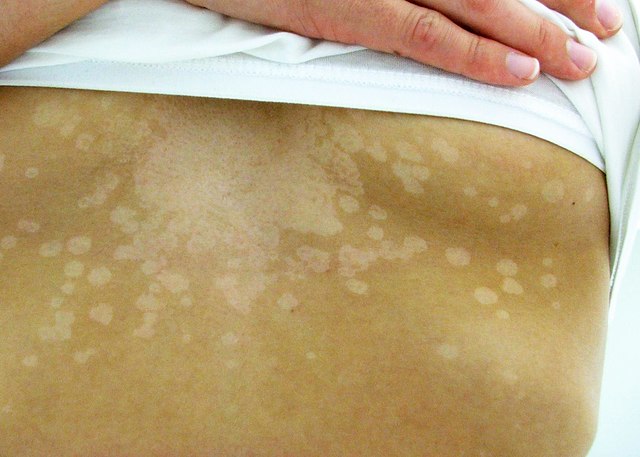
- Small, round patches of skin that become lighter or darker than the surrounding skin
- Mild itching
- Patches that become more noticeable after sun exposure due to the unaffected skin tanning while the infected area does not
Diagnosis and Tests
This condition is not dangerous, but it can cause significant distress due to its appearance. Healthcare providers can diagnose tinea versicolor using a couple of different skin tests:
Microscopic Examination of Skin Scrapings
This involves gently scraping off a small bit of skin from one of the discolored patches. The collected skin cells are then combined with a drop of a specialized solution. This solution helps make the fungus more visible to the examiner. The skin sample is then examined under a microscope to look for signs that confirm the diagnosis of tinea versicolor.
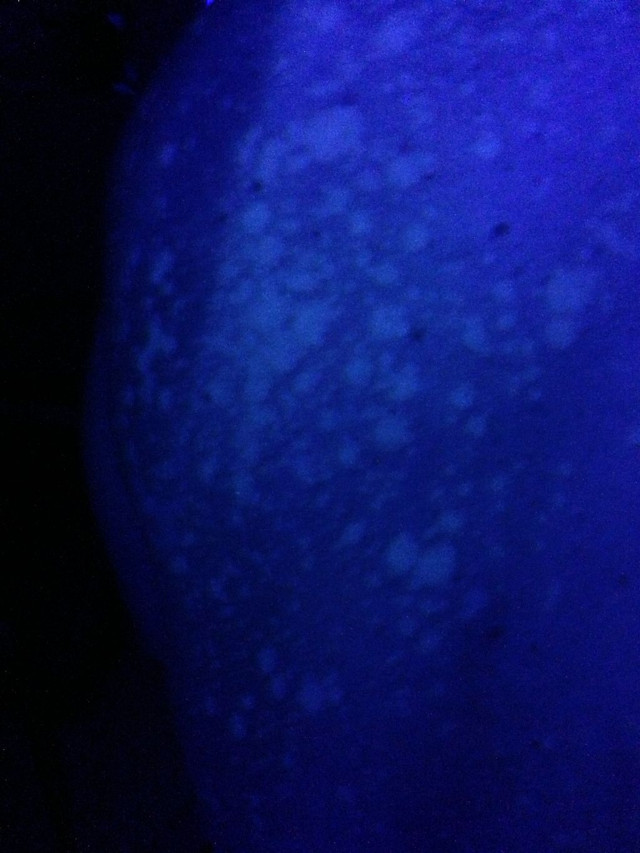
Wood's Lamp Examination
A Wood's lamp is a handheld device that emits ultraviolet (UV) light. When the skin is examined under this light in a dark room, areas affected by certain fungi, including the yeast that causes tinea versicolor, will glow with a yellow-green color.
Management and Treatment
After confirming the diagnosis, healthcare providers can recommend appropriate treatment options, which typically include topical antifungal medications. In more severe cases, or when topical treatments fail, oral antifungal medications might be prescribed.
It's important to note that while treatment can clear up the infection, the skin discoloration may take several months to resolve and may recur, especially in warm, humid climates.

Prevention
Preventive measures include:
- Using medicated cleansers or soaps containing antifungal agents
- Avoiding excessive heat and sweating
- Applying sun protection to prevent skin discoloration contrast
- Maintaining good hygiene to help you prevent yeast growth even before it shows some early signs.
- Reducing sweating to discourage the development of moisture that’s one of the breeding grounds of the yeast that causes this condition
- Avoiding oily lotions to ensure that dirt and other debris will not stay trapped in different parts of your skin
Living With Tinea Versicolor
With proper treatment, most individuals recover fully from tinea versicolor. However, skin discoloration may persist for weeks or months, and the condition can recur, especially in warm, humid climates. Even if this is the case, you don’t have to worry because this condition is temporary. You also don’t have to worry about the discoloration leading to permanent scars because this doesn’t usually happen if you have the condition.
If you have concerns about the length of treatment and how to manage your expectations, consult your physician. They will guide you through the best course of action to take to help you cope better with your situation.
For those with a history of the condition, ongoing management may be necessary to prevent recurrence. This can include having a regular skincare routine, using medicated soaps, and staying vigilant during warmer months when the yeast is more likely to overgrown.
(Editor's note: This article is not a substitute for medical advice. It's always best to see a doctor to receive an accurate diagnosis.)



